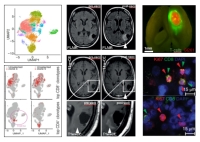
Clinical Cooperation Unit Neuroimmunology and Brain Tumor Immunology
Prof. Dr. med. Michael Platten
The central nervous system (CNS) is considered an immune privileged organ, where immune responses are tightly controlled through an intensive cross-talk with the peripheral immune system despite the blood-brain barrier. Imbalance of such immune control is a hallmark of CNS autoimmunity, while on the other hand, active immunosuppression in the tumor microenvironment of CNS tumors like gliomas hampers effective antitumor immune responses. Our group aims at developing and improving immune therapeutic approaches to target brain tumors by understanding molecular mechanisms of immunosuppression and exploiting novel immunotherapeutic treatment modalities. With expertise in comprehensive cellular and imaging-based analysis of tumor microenvironments, transcriptomics, and immunoreceptor profiling and utilization, and using clinical samples and mouse models, we strongly focus on clinical translation.
In the past years we have identified immunosuppressive functions and mechanisms of key metabolites that are produced by brain tumors. The discovery that TDO-derived tryptophan metabolites (kynurenines) drive growth of brain tumors and immunosuppression via the activation of the aryl hydrocarbon receptor (AHR) opened the way to novel therapeutic targets and implied further questions which we currently address using tumor models. A central goal is the identification of drugs interfering with tryptophan catabolism as potential therapeutics for malignant glioma. Our findings that IDH-mutant glioma cell-derived 2HG actively and directly inhibits adaptive cellular and innate immune responses by affecting immune cell function in the tumor microenvironment pave the way towards novel concepts of immunotherapeutic combination treatments which we are currently investigating in preclinical animal glioma models and chaperoning on their clinical translation.
A second line of investigations addresses the discovery of novel target antigens and T cell receptors for targeted immunotherapy of gliomas. Using an MHC-humanized syngeneic mouse tumor model we have shown therapeutic efficacy of an IDH1 mutation-specific vaccine, providing the first evidence that mutation-specific T helper cell responses are capable to control solid tumors. On that basis we have successfully completed a phase I clinical trial to test immunogenicity and tolerability of this vaccine in brain tumor patients, showing strong immunogenicity, enhanced pseudoprogression as a surrogate marker for immune cell infiltration and successful anti-tumor immune response, and IDH1 mutation-specific T cells infiltrating into this post-vaccine lesion. Ongoing projects now focus on identification of further mutational antigens for specific immunotherapy and on specific TCR discovery for use in transgenic T cell therapy for glioma patients. Here, our main focus lays on long-neglected CD4+ T helper cells. In this regard, a workflow for the development of a patient-specific targeted immunotherapy for patients with gliomas based on mutanome analyses and T cell receptor identification as well as an MHC-humanized mouse glioma model for preclinical testing have been developed. Bioinformatics-based approaches for tumor-infiltrating reactive T cell selection for such TCR discovery based on high throughput state-of-the-art single cell RNA, single cell VDJ, as well as TCRbeta deep sequencing, are boosting these processes and progress.