Division of Medical Physics in Radiation Oncology
Prof. Dr. Oliver Jäkel
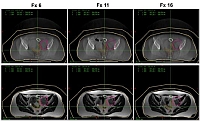
Typical image sequence generated in our shuttle based MR-guidance study at DKFZ: Conventional cone beam CT images of a patient with lymph node metastases from an anal carcinoma taken in fraction 6, 11 and 16 (top) compared to T2 -weighted MR-images taken at the same day prior to radiotherapy.
© dkfz.de
Research in our Division is dedicated on improvements of radiotherapy techniques using photons and ion beams. In the ongoing projects we focus on the adaption of the treatment to dynamic changes of target volumes and organs at risk under therapy, due to therapeutic response, organ motion or patient setup. Image-guided and time-adapted therapy is being developed to combine high precision dose delivery with online imaging of 3D anatomy and online monitoring of 3D dose distributions.
The Division is furthermore investigating the potential of integrating also functional imaging into treatment planning and adaption, aiming at boosting radio-resistant tumor sub-compartments and avoiding radiosensitive normal tissue structures. Establishing mathematical and biological models of tumor and normal tissue response is another tool to optimize treatment schemes and techniques. One of the strengths of the Division is the direct transfer of software and hardware development prototypes into clinical applications in close collaboration with the Radiation Oncology Clinical Cooperation Unit. The Division is also active in testing and establishing adequate quality assurance measures. This includes a cooperation with our national standard laboratory for dosimetry, PTB, which aims at developing novel and highly accurate dose measurement systems for scanned ion beams based on water calorimetry.
Finally, the division developed a system of courses for continuing education in medical physics and radiation oncology, which are based on an E-learning platform to establish a blended-learning approach.
FUTURE OUTLOOK
Current research and development projects concentrate on the development of MR guided radiotherapy in order to allow a simultaneous monitoring of patient anatomy during treatment. In order to use this information, many new tools have to be developed, including fast dose calculation algorithms, strategies to allow for a fast adaptation of the treatment plan and methods to still ensure the quality of this new treatment concept. Together with the University Hospital and the departments for radiology and medical physics in radiology, the department is part of the Heidelberg consortium for MR-guided Radiotherapy, which successfully applied for funding of a prototype installation of a new hybrid machine in Heidelberg with DFG. The system is currently under installation and expected to start clinical operation in early 2018. New projects will be focused on the topic MR guided radiotherapy using adaptive concepts.
In the field of ion beam therapy the focus is on developing effective strategies to use the in-room X-ray imaging for improved volumetric imaging, which is needed for treatment adaption. To support biologically guided radiotherapy at DKFZ, we pursue the development of a unified treatment planning and optimization platform that specifically takes into account the information provided by functional imaging. In heavy ion therapy, new detector systems are being investigated, like a novel hybrid detector to correlate e.g. DNA damage in single cells with the traversing ion tracks or a secondary particle monitor, which may allow in-vivo tracking of the applied ion beam dose in patients.
Another important research area focuses on the radiobiology of ion beams and the benchmarking of radiobiological models. This is done in various animal models, which allow for a pre-clinical assessment of the biological effectiveness of various ion beams in tumors and normal tissues under various conditions.
In order to support also the clinical implementation of novel techniques, we are furthermore developing novel strategies for treatment plan optimization, like probabilistic concepts that allow for an inclusion of uncertainties in the optimization process. These developments are being implemented in an open source treatment planning toolkit (MatRad), which also serves as a platform for cooperation projects and teaching activities.
Finally, we have a group involved in designing new hardware for the support of radiotherapy. This includes novel concepts for patient fixation, sophisticated phantom design for dedicated QA applications, but also solutions for special requirements arising from the combination of MR imaging in the radiotherapy process, like MR-compatible systems for fixation or the positioning of MR-coils in the patient fixation devices.

