Individual cancer cells that break away from the original tumor and circulate through the blood stream are considered responsible for the development of metastases. These dreaded secondary tumors are the main cause of cancer-related deaths. Circulating tumor cells (CTCs) detectable in a patient’s blood are associated with a poorer prognosis. However, up until now, experimental evidence was lacking as to whether “stem cells" that lead to metastases can be found among CTCs.
“We were convinced that only a very few of the various circulating tumor cells are capable of forming a secondary tumor in a different organ," says Prof. Andreas Trumpp, a stem cell expert. “Many patients do not develop metastases even though they have cancer cells circulating through their blood." Trumpp is head of DKFZ’s Division of Stem Cells and Cancer and director of the Heidelberg Institute for Stem Cell Technology and Experimental Medicine (HI-STEM) at DKFZ. “Metastasis is a complex process and cancer cells need to have very specific properties for it," he says. “Our hypothesis was that the characteristics of cancer stem cells, which are resistant to therapy and very mobile, are best suited.“
Irène Baccelli from Trumpp’s team developed a transplantation test for the experimental detection of metastasis-initiating cells. In collaboration with Prof. Andreas Schneeweiss from the National Center for Tumor Diseases (NCT) Heidelberg, along with colleagues from the Institute of Tumor Biology in Hamburg and the Institute of Pathology of Heidelberg University Hospitals, the researchers analyzed the blood of more than 350 breast cancer patients. Using specific surface molecules, Baccelli isolated circulating tumor cells from the blood and directly transplanted them into the bone marrow of mice with defective immune systems. “Bone marrow is a perfect niche for tumor sells to colonize," Trumpp explains. After more than one hundred transplantations, metastases started forming in the bones, lungs and livers of some of the animals.
This proved that CTCs do contain metastasis stem cells – even though their frequency is apparently low. What characterizes these cells? To define their molecular properties, the researchers analyzed the surface molecules of the CTCs that had led to metastases after transplantation.
Three molecules characterize the metastasis stem cell
In a systematic screening process, Baccelli first isolated cells carrying a typical breast cancer stem cell protein (CD44) on their surface from the CTCs. This protein helps the cell to settle in bone marrow. Next, the researchers screened this cell population for specific surface markers which help the cells to survive in foreign tissue. These include, for example, a signaling molecule (CD47) that protects them from attacks by the immune system, and a surface receptor that enhances the cells’ migratory and invasive capabilities (MET).
Using a cell sorter, the researchers were then able to isolate CTCs which simultaneously exhibit all three characteristic molecules (CD44, CD47, MET). Another round of transplantation tests showed that these were in fact the cells from which the metastases originated.
Depending on the patient, cells exhibiting all three surface molecules (“triple-positive" cells) made up between 0.6 and 33 percent of all CTCs. “It is interesting that only cells with the stem cell marker CD44 carry the combination of the other two surface molecules," said Irène Baccelli. “It looks like the triple-positive cells are a specialized subtype of breast cancer stem cells circulating in the blood."
Triple-positive cells as prognostic biomarkers
Are the triple-positive cells a more precise biomarker of breast cancer progression than the number of CTCs alone? In a small patient group, the researchers observed that as the disease advances, the number of triple-positive cells increases, but the total number of CTCs does not. In addition, patients with very high numbers of triple-positive cells had particularly high numbers of metastases and a much poorer prognosis than women in whom only a few metastasis-inducing cells were detected. “On the whole, triple-positive cells seem to have a substantially higher biological relevance for disease progression than previously studied CTCs," Andreas Schneeweiss explains. The researchers plan to confirm these new results in a large study.
Andreas Trumpp considers it good news that metastasis-initiating cells are characterized by the two proteins CD47 and MET. Therapeutic antibodies that target CD47 and inhibit its functions are already being developed. A substance inhibiting the activity of the MET receptor has already been approved and shows good effectiveness in treating a type of lung cancer. The substance may also help breast cancer patients with detectable metastasis-inducing cells. “The triple-positive cells we have found turn out to be not only a promising biomarker of disease progression in breast cancer but also a prospect for potential new therapeutic approaches for treating advanced breast cancer," says Andreas Trumpp.
Irène Baccelli, Andreas Schneeweiss, Sabine Riethdorf, Albrecht Stenzinger, Anja Schillert, Vanessa Vogel, Corinna Klein, Massimo Saini, Tobias Bäuerle, Markus Wallwiener, Tim Holland-Letz, Thomas Höfner, Martin Sprick, Martina Scharpff, Frederik Marmé, Hans Peter Sinn, Klaus Pantel, Wilko Weichert and Andreas Trumpp: Identification of a population of blood circulating tumor cells from breast cancer patients that initiates metastasis in a xenograft assay. Nature Biotechnology 2013, DOI: 10.1038/nbt.2576
A picture for this press release is available at:
ctc-induced-bone-xenograft.jpg
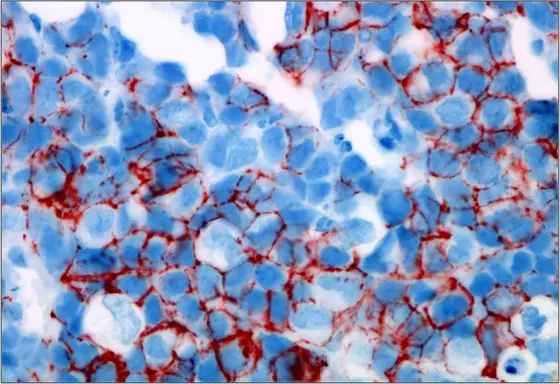
Circulating tumor cells isolated from the blood of breast cancer patients form a metastatic tumor in the bone marrow of mice. The stem cell marker CD44 is dyed red.
Source: Irène Baccelli, DKFZ