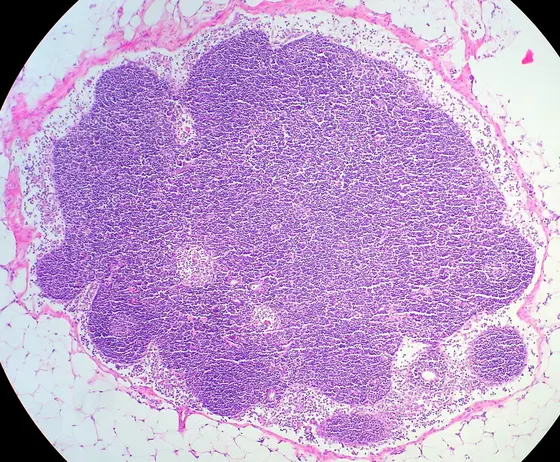
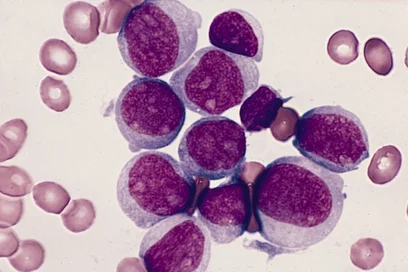
Lymph nodes are central hubs of the immune system and play a vital role in defending against infections and tumors. For this to function properly, immune cells (B cells and T cells) must be precisely organized spatially within the lymph node tissue, for example in so-called B-cell follicles and T-cell zones. This is controlled by stromal cells (non-hematopoietic supporting cells). They release signaling molecules, thereby generating guidance signals that immune cells use to find their designated locations within the lymph node.
In B-cell lymphomas, the internal organization of the lymph node tissue is disrupted in very different ways depending on the disease: While in slow-growing lymphomas, such as follicular lymphoma (FL), the basic tissue structure remains intact, the spatial organization in aggressive lymphomas, such as diffuse large B-cell lymphoma (DLBCL), breaks down completely. Why these typical growth patterns arise has been largely unclear until now.
In the current study, the researchers succeeded for the first time in systematically mapping these processes in human lymph nodes. Using single-cell analyses and spatial tissue mapping, they were able to trace which factors cause the lymph node architecture to increasingly disintegrate in lymphoma diseases.
The data show that stromal cells are the “architects” of the lymph node. The researchers were able to demonstrate that key signaling pathways in specialized stromal cells undergo fundamental changes in lymphoma, causing the spatial organization of the lymph node to gradually collapse. These changes in stromal cells are reflected in the growth patterns of lymphomas: While in FL the relative sizes of B-cell follicles and T-cell zones shift, the areas remain largely spatially separated; in DLBCL, however, key regulatory signals—and thus the tissue structure—are largely lost.
The study identifies an inflammatory vicious cycle as the driving mechanism: As part of the immune response in the tumor microenvironment, T cells produce pro-inflammatory signaling molecules, known as interferons, which cause stromal cells to switch their production of signaling molecules (chemokines): Instead of structure-defining signals, inflammatory chemokines dominate, which in turn attract further inflammatory cells. The loss of lymph node organization in lymphomas is therefore not a passive effect of tumor growth, but is actively driven by inflammatory processes in the tumor microenvironment.
In patients, this reprogramming of stromal cells is associated with poorer survival outcomes. The researchers were able to demonstrate in large patient cohorts that a loss of structuring chemokines is associated with an unfavorable prognosis.
These findings also open the door to new potential therapeutic approaches. “Our results could be very important for the development of new therapies and diagnostic procedures,” said Daniel Hübschmann of the DKFZ.
Source: Press release from the University Hospital Düsseldorf
Publication:
Felix Czernilofsky et al.: Reprogramming of stroma-derived chemokine networks drives the loss of tissue organization in nodal B-cell lymphoma
Nature Cancer 2026, DOI: 10.1038/s43018-026-01136-z