Metastatic tumors, the dreaded “daughter tumors“, form when cancer cells break away from a tumor and migrate via the lymph and the bloodstream in order to finally settle at some distant site in the body. However, the quantity of circulating cancer cells in the body is not the only factor that determines a patient's risk of developing metastatic sites. “Some patients display high quantities of circulating tumor cells and have no or only a few metastatic sites while in others who suffer from many metastases, hardly any migrating tumor cells can be found,“ said Mathias Heikenwälder from the German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ) in Heidelberg.
The team led by Heikenwälder has therefore taken a closer look at the properties of migrating cancer cells. In human cancer cells as well as in patients with different types of cancer, and also in mice, they observed that a portion of the circulating cancer cells exhibit a specific polarity. “Under the microscope, this looks as if the cells had a kind of nose,“ Heikenwälder described. Two cytoskeletal proteins called ezrin and merlin play a key role in the formation of this nose. Furthermore, the scientists also found that the number of freely circulating tumor cells exhibiting this special polarity correlates with the risk of developing metastasis, both in human tumor cell lines and in mice.
“This polarity seems to help the free cancer cells return from the blood vessels into body tissue,“ explains Anna Lorentzen, who is the first author of the publication. With the polarized end, i.e., with the nose, the cells attach to the endothelial layer lining the interior of the vessels. Subsequently, the pole is shifted to the side facing the attachment site and the tumor cell migrates through the endothelial layer into the tissue.
As a cross-check, the researchers used a cell-biological trick to block polarization of the circulating cells. Both in culture and in mice, the manipulated cells were no longer able to attach efficiently to endothelial cells.
With this discovery, the DKFZ researchers have not only found a new mechanism promoting the formation of metastatic sites. “We also have found a link that might in future be used to better predict and even reduce the risk for metastasis in cancer patients,“ Heikenwälder stressed.
Anna Lorentzen, Paul F. Becker, Jan Kosla, Massimo Saini, Kathrin Weidele, Paolo Ronchi, Corinna Klein, Monika J. Wolf, Felix Geist, Bastian Seubert, Marc Ringelhan, Daniela Mihic-Probst, Knud Esser, Marko Roblek, Felix Kuehne, Quentin Müller, Kathleen Schuck, Sebastian Lange, Daniel Hartmann, Saskia Spaich, Olaf Groß, Jochen Utikal, Sebastian Haferkamp, Martin R. Sprick, Amruta Damle-Vartak, Nachiket Vartak, Alexander Hapfelmeier, Norbert Hüser, Ulrike Protzer, Andreas Trumpp, Dieter Saur, Christoph A. Klein, Bernhard Polzer, Lubor Borsig and Mathias Heikenwalder: Single cell polarity in liquid phase facilitates tumour metastasis. Nature Communications, 2018, DOI: 10.1038/s41467-018-03139-6
A picture is available for Download:
ezrin.jpg
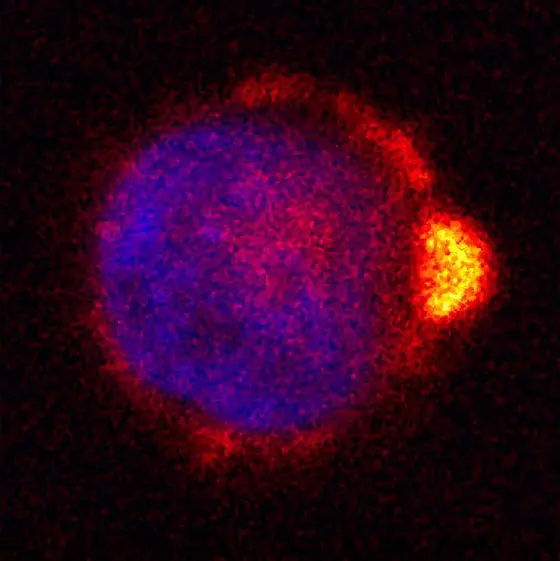
Picture Caption: A human melanoma cell exhibits a specific polarity which helps attaching to the endothelial layer of the blood vessel (ezrin stained in orange)
Note on use of images related to press releases
Use is free of charge. The German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ) permits one-time use in the context of reporting about the topic covered in the press release. Images have to be cited as follows: “Heikenwälder/DKFZ“
Distribution of images to third parties is not permitted unless prior consent has been obtained from DKFZ's Press Office (phone: ++49-(0)6221 42 2854, E-mail: presse@dkfz.de). Any commercial use is prohibited.