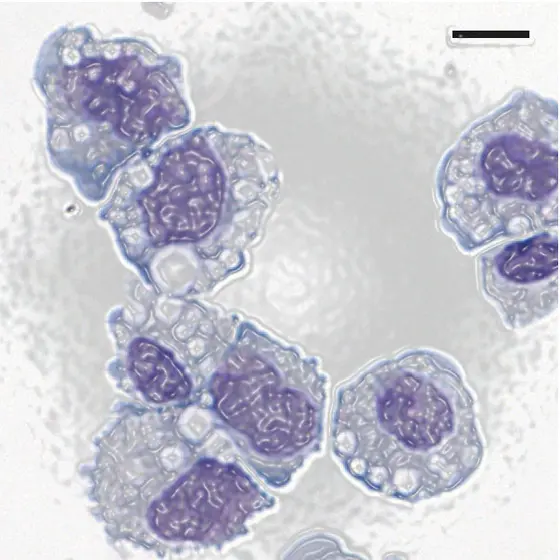
Macrophages (Greek: “big eaters") are cells of the immune system. In tissues, they recognize both foreign invaders (pathogens) and aged cells of the body, which they engulf and digest. Macrophages are specific to different types of tissue. For example, they are called Kupffer cells in the liver, osteoclasts in the bone, alveolar macrophages in the lungs, and microglia in the brain.
These cells are classified as blood cells because they can be cultivated in the lab from specific white blood cells called monocytes. “Therefore, it has been regarded as established that macrophages also arise from stem cells in the bone marrow," says Hans-Reimer Rodewald from the German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ). “Our new results now challenge this textbook view."
The first blood cells are generated in the yolk sac, a special tissue that provides nutrients to the fetus during early embryonic development and later disappears. When that happens the fetal liver first takes over the vital task of providing a continuous supply of new red and white blood cells; later the bone marrow steps in. “We wanted to know whether this also holds true for macrophages that reside in tissue," says Rodewald, “because evidence suggested that these special cells might also have other origins."
The scientists in Rodewald’s team labeled progenitor cells with a fluorescent protein in order to identify the point in development when macrophages form and the tissue in which this happens. To dye the cells, they used a special gene switch that had been developed by Katrin Busch, a PhD student in Rodewald’s lab. “We could see that the tissue-resident macrophages form very early in the embryonic phase from progenitors in the yolk sac,“ says Kay Klapproth, one of the two first authors of the study. “This runs counter to what we have believed until now. It shows that macrophages are not supplied from the bone marrow, but renew themselves independently in the tissue where they reside."
“This holds true for macrophages in normal healthy tissue," says Rodewald. “In cases where there is a higher demand for the cells, due to inflammations or a depletion of macrophages, monocytes from the bone marrow appear to be able to provide more tissue macrophages." It is still unclear whether these substitute macrophages carry out the same tasks as the “conventional" macrophages.
The scientists now plan to determine how the original macrophages from the yolk sac are distinguished from “emergency" macrophages called up from the bone marrow. “In certain types of cancer, macrophages might contribute to the spread of tumor cells," Klapproth says. “In other cases, they are believed to have tumor-inhibiting functions." At present, it is still unclear whether these contradictory functions might be linked to the different origins of the macrophages. In cancer treatment, it would be desirable to be able to fight “harmful" macrophages and to selectively activate “useful" cells. However, it is not yet possible to distinguish the two cell types from each other. “In the future, it would be exciting if our new findings could be used to distinguish different classes of macrophages based on their origins," Rodewald says.
Elisa Gomez Perdiguero, Kay Klapproth, Christian Schulz, Katrin Busch, Emanuele Azzoni, Lucile Crozet, Hannah Garner, Celine Trouillet, Marella F. de Bruijn, Frederic Geissmann, Hans-Reimer Rodewald: Tissue-resident macrophages originate from yolk-sac-derived erythro-myeloid progenitors. Nature 2014, DOI 10.1038/nature13989