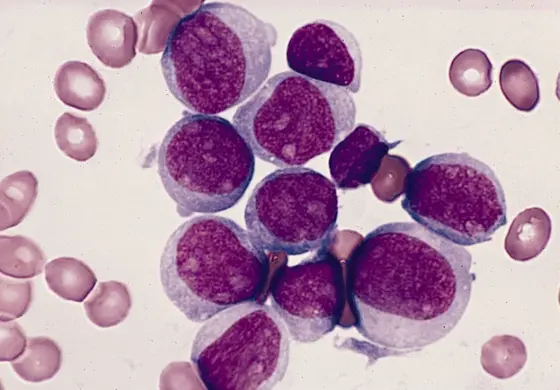
Acute myeloid leukemia (AML) is the most common and very aggressive form of blood cancer in adults. Until recently, only high-dose chemotherapy was available to treat the disease. But for about half of those affected, especially elderly or frail individuals, this distressing treatment is out of the question.
The agent Venetoclax has been approved for several years. The survival of AML cells depends on certain proteins that suppress programmed cell death - apoptosis. Venetoclax specifically inhibits the anti-apoptotic protein BCL-2, which leukemia cells use to protect themselves from cell death, thereby keeping AML in check. A combination of Venetoclax and the epigenetic drug 5-Azacitidine (Ven/Aza) is comparatively well tolerated and has significantly improved the treatment of patients for whom high-dose chemotherapy is not an option.
Therefore, it is currently being investigated whether this drug combination is also suitable as a so-called first-line treatment in younger or physically fit AML patients, which would spare them the need for high-dose chemotherapy. However, not every AML patient responds to the drug combination. In some cases, the leukemia cells are resistant from the start. “Until now, there have been no predictive markers that can reliably predict a response to Venetoclax,“ says Andreas Trumpp, head of department at the German Cancer Research Center (DKFZ) and director of HI-STEM in Heidelberg.
Together with colleagues from Heidelberg University Hospital, Alexander Waclawiczek, Aino-Maija Leppä and Simon Renders in the Trumpp team now looked for characteristics in blood and bone marrow samples from Ven/Aza-treated AML patients that correlate with response to therapy. The researchers found that a small population of cells that exhibit characteristics of leukemia stem cells is responsible for therapy response. If these cells express a specific combination of proteins in the BCL-2 family, the Ven/Aza combination can trigger programmed cell death in the leukemia stem cells, halting AML.
BCL-2, a known inhibitor of apoptosis, is a member of a family of proteins involved in the regulation of programmed cell death. The Heidelberg research team found that it is not only the amount of BCL-2 in the leukemia stem cells that determines the Ven/Aza response, but that it is the quantitative ratio of certain members of the BCL-2 family that is important. Based on this observation, they derived the so-called “MAC score“ (“Mediators of Apoptosis Combinatorial score“), which expresses the quantity ratio of the proteins BCL-2, BCL-xL and MCL-1 in the AML stem cells and can be determined by flow cytometry. The higher the score, the longer the treatment success lasted.
“We can thus provide an inexpensive test that gives reliable information after just a few hours as to whether an AML is responding to Ven/Aza and thus whether the stressful high-dose chemotherapy can be avoided,“ says study leader Andreas Trumpp. The test can be performed in any well-equipped hematology laboratory to determine the best possible form of treatment for leukemia patients.“ Together with Carsten Müller-Tidow at Heidelberg University Hospital V, the results will be further evaluated in prospective clinical studies before the test can find its way into the routine care of AML patients.
Alexander Waclawiczek, Aino-Maija Leppä, Simon Renders, Karolin Stumpf, Cecilia Reyneri, Barbara Betz, Maike Janssen, Rabia Shahswar, Elisa Donato, Darja Karpova Vera Thiel, Julia M. Unglaub, Susanna Grabowski, Stefanie Gryzik, Lisa Vierbaum, Richard F. Schlenk, Christoph Röllig, Michael Hundemer, Caroline Pabst, Michael Heuser, Simon Raffel, Carsten Müller-Tidow, Tim Saue and Andreas Trumpp: Combinatorial BCL-2 family expression in Acute Myeloid Leukemia Stem Cells predicts clinical response to Azacitidine/Venetoclax
Cancer Discovery 2023, DOI: doi.org/10.1158/2159-8290.CD-22-0939
* The Heidelberg Institute for Stem Cell Technology and Experimental Medicine (HI-STEM) gGmbH was founded in 2008 as a public-private partnership between the DKFZ and the Dietmar Hopp Foundation.