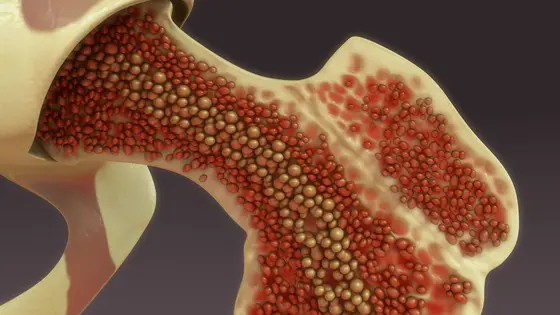
Our blood contains many different types of cell that are involved in our immune system, in transporting oxygen, and in healing wounds. Simon Haas of the BIH, the MDC, and HI-STEM explains that our bodies dispose of old cells and form about a billion new ones every day: “It might even be more than that, depending on what the individual needs. A COVID patient, for instance, will need more immune cells to help them fight off the infection. And all those new cells come from the stem cells in our bone marrow. They keep doing their job for our entire lives.“
Passive and active protection for stem cells
But because these stem cells have to produce so many cells, their genome needs extremely good protection against damage. “Any errors will be passed on to the daughter cells and multiplied,“ says Haas. Researchers have therefore long been trying to track down the mechanism that ensures stem cells only rarely mutate. One of them came to light a while ago: “Within the bone marrow, the stem cells reside in a stem cell niche that protects them from harmful environmental factors,“ says Andreas Trumpp, director of HI-STEM and head of the Stem Cells and Cancer Division at DKFZ in Heidelberg. “They sort of lie dormant there and only wake up when they're needed. It's a very reliable system. The protection only starts to decline in old age, which is why leukemia sadly occurs more frequently in older people.“
But this passive protection is clearly just one part of the secret of our unscathed stem cells. Haas and his team have now discovered that occasionally mutated stem cells are apparently recognized and eliminated before they can do any damage. “The stem cell niche contains immune cells called T cells, and they regularly check which proteins are being presented on the surface of the stem cells,“ says Haas. “If the immune cells detect cancerous changes in a stem cell, they activate it and drive it out of the niche.“
Single-cell technologies show that stem cells communicate with T cells
The researchers discovered this interaction between the T cells and the stem cells rather by chance. Pablo Hernández-Malmierca, the lead author of the study, was investigating the stem cells using gene expression analyses and single-cell technologies. “That's how we learned that the stem cells in bone marrow produce all the proteins needed for communicating with T cells in the bone marrow niche.“
The team was most surprised to find that the stem cells appear to use signaling molecules that only a few specialized types of cell deploy for communicating with T cells. “The only cells that communicate via MHC class II molecules on their surface are professional antigen-presenting cells,“ says Haas. “This then triggers an immune response that kills infected or mutated cells. At first we couldn't believe that stem cells in bone marrow were also using this specific pathway.“ To check whether the stem cells actually used the MHC II molecules they were producing, second lead author Dominik Vonficht brought stem cells and T cells together in a petri dish.
“We discovered that the mutated stem cells activate the T cells by presenting fragments of their mutated proteins on the MHC II molecules. We also saw that the T cells activate the stem cells by using their T cell receptor to bind to the MHC II molecules. So the communication works in both directions,“ says Hernández-Malmierca. “The activated stem cells do divide, but this time both daughter cells differentiate to form blood cells – instead of one remaining a stem cell. This removes the danger of a mutated stem cell continuing to produce mutated offspring.“
Rewriting the textbooks
The researchers also showed that the stem-cell safety mechanism functions via the MHC II pathway in mice. “We bred mice with two different types of stem cell: Half the stem cells were healthy, and the other half presented fragments of a diseased protein on their surface via the MHC II molecule. When we gave the mice T cells whose receptors recognized the protein, the mutated stem cells gradually disappeared from the bone marrow, leaving only the healthy ones. This protected the mice from developing leukemia,“ explains Alexandra Schnell of Harvard Medical School. Analysis of clinical data showed that the newly discovered mechanism also removes problematic stem cells to prevent mutations in humans.
Haas – whose research group is part of the joint focus area “Single Cell Approaches for Personalized Medicine“ at the BIH, Charité, and the MDC – is delighted that the new technologies are rewriting the textbooks. “It used to be taken as given that only dendritic cells, macrophages, and B cells have MHC II molecules and present antigens. We're very surprised to have discovered that blood stem cells in bone marrow also use this very same mechanism to communicate with T cells – and I suspect that will also be the case for most of our colleagues.“ “In the future, the findings could help to diagnose and possibly eliminate the first degenerate cells before cancer develops,“ adds Andreas Trumpp.
Hernandez-Malmierca P, Vonficht D, Schnell A, Uckelmann HJ, Bollhagen A,
Mahmoud MAA, Landua SL, Van der Salm E, Trautmann CL, Raffel S, Grunschlager
F, Lutz R, Ghosh M, Renders S, Correia NC, Donato E, Dixon KO, Hirche C, Andresen C, Robens C, Werner PS, Boch T, Eisel D, Osen W, Pilz F, Przybylla A, Klein C, Buchholz F, Milsom MD, Essers MAG, Eichmuller SB, Hofmann WK, Nowak D, Hubschmann D, Hundemer M, Thiede C, Bullinger L, Muller-Tidow C, Armstrong SA, Trumpp A, Kuchroo VK, Haas S: Antigen presentation safeguards the integrity of the hematopoietic stem cell pool
.
CELL Stem Cell 2022, DOI: doi.org/10.1016/j.stem.2022.04.007