Liver cancer is the sixth most common type of cancer in the world, but the fourth most common cause of death from cancer. That is mainly due to the fact that liver cancer is often not detected until a late stage. Although various therapies are available to treat advanced-stage disease, they can usually only temporarily halt progression of the disease. Immunotherapies – known as checkpoint inhibitors – are effective in around a quarter of patients. Up to now, it was unclear which patients were likely to benefit from this treatment and which were not.
The development of liver cancer is driven by chronic inflammation, which can be due to chronic hepatitis B or C infection or alcohol abuse. An unhealthy lifestyle can also contribute to development of the disease: too many calories, too little exercise, and excessive body weight lead to fatty liver. In turn, this may result in non-alcoholic steatohepatitis or NASH – a hotbed for liver cancer.
“Fatty liver and NASH are taking on pandemic proportions across the globe,“ explained Mathias Heikenwälder from the German Cancer Research Center (DKFZ). Heikenwälder, a metabolic specialist, investigated the presumption that the different triggers of cancer-promoting inflammation might influence whether or not immunotherapy is effective.
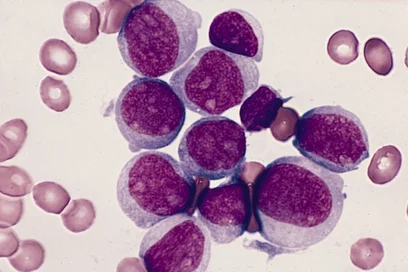
Mice fed a high-fat diet develop fatty liver and subsequently, like many obese patients, suffer from NASH. In the livers of these animals, the researchers observed an unusually high number of certain T cells carrying the PD1 molecule on their surface (CD8+PD-1+ T cells). Yet these special cells did not protect the animals against the development of liver cancer, but instead appeared to exacerbate the inflammatory tissue damage and surprisingly to actually promote the development of cancer.
The number of harmful T cells increased even further if NASH mice suffering from liver cancer were treated using a checkpoint inhibitor. The liver damage became worse and more tumors occurred. In contrast, in mice without NASH, treatment using checkpoint inhibitors was able to suppress liver cancer, as expected.
“The metabolically activated T cells in the inflamed liver are not only unable to fight liver cancer. They are also autoaggressive and actually drive cancer development. They even increase in number during treatment with the checkpoint inhibitors,“ Heikenwälder explained.
In collaboration with Percy Knolle and his research team at TU München, Heikenwälder was able to reveal the mechanisms that lead to this autoaggressive disease. The results were also published at the same time in Nature*.
Heikenwälder's results contradict one of the tenets of immunotherapy, according to which the more T cells there are in a tumor, the more likely immunotherapy is to be successful. “That is not true in patients with fatty liver-driven liver cancer,“ Heikenwälder remarked.
An analysis of various patient cohorts with inflammatory liver disease compared with healthy controls showed that these results are not only relevant to obese mice. In the diseased livers, the researchers found T cells whose molecular profile corresponded to the harmful autoaggressive T cells in the NASH mice.
“For us, that was an indication that checkpoint inhibitors might not work in patients with liver cancer caused by inflammatory fatty liver disease,“ Heikenwälder continued.
In order to support their hypothesis, the research team evaluated several clinical studies on the efficacy of checkpoint inhibitors in liver cancer. A total of around 2,000 patients were enrolled in these studies. In the group of patients with virus-associated tumors, the checkpoint inhibitors improved the cancer survival rate. However, patients with NASH-related liver cancer did not benefit from the treatment. On the contrary: their survival time was considerably shorter than that of patients with virus-associated liver cancer who received exactly the same treatment.
“For the first time, we have identified a biomarker – NASH-related liver cancer – that can help physicians assess whether or not a patient will benefit from immunotherapy,“ Heikenwälder explained, adding a further important conclusion from the current results: Many thousands of patients with various types of cancer are treated every year using checkpoint inhibitors. Very many of them are overweight – which increases the likelihood of inflammatory fatty liver disease. In these patients, there might be a risk that immunotherapy further activates the autoaggressive T cells in the liver. “That once again underlines how important it is to keep a close eye on liver function in cancer patients being treated with checkpoint inhibitors.“
Dominik Pfister et al.: NASH precludes anti-tumor surveillance in immunotherapy-treated hepatocellular carcinoma. Nature 2021, DOI: 10.1038/s41586-021-03362-0
* Dudek et al.: Auto-aggressive CXCR6+ 1 CD8 T cells cause liver 2 immune pathology in NASH. Nature 2021, DOI: 10.1038/s41586-021-03362-0
A picture is available for Download: www.dkfz.de/de/presse/pressemitteilungen/2021/bilder/210319_DKFZ_Cover_Nature_Leber.jpg
Caption: Inflammatory fatty liver disease and liver cancer - an artistic illustration
Note on use of images related to press releases
Use is free of charge. The German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ) permits one-time use in the context of reporting about the topic covered in the press release. Images have to be cited as follows: “Source: Peter von Walter / DKFZ“.
Distribution of images to third parties is not permitted unless prior consent has been obtained from DKFZ's Press Office (phone: ++49-(0)6221 42 2854, E-mail: presse@dkfz.de). Any commercial use is prohibited.