Cytokines such as interleukins and interferons are endogenous messenger proteins that stimulate the immune system to fight infection and tumors. Researchers have been trying for decades to use the immunostimulatory properties of cytokines to treat cancer. Progress has been made in recent years in infiltrating tumors with cytokines by attaching them to antibodies that target cancer-specific proteins. One of the problems in the clinical development of these immunocytokines are the severe side effects caused by uncontrolled immune activation, however. “Cytokines are toxic in larger quantities and activation is unfortunately nonspecific if they are fused to antibodies in the blood without being attached to the tumor,“ explained DKTK Professor and physician Helmut Salih, head of the Clinical Cooperation Unit Translational Immunology at Tübingen University Hospital. “This can lead to a real cytokine 'storm', which causes fever, exhaustion and sometimes even cardiovascular shock.“
Salih and his colleague Gundram Jung, head of the Experimental Antibody Therapy section at Tübingen University, thus designed a new, modified form of immunocytokines (MICs). They attached interleukin IL-15 to an antibody that recognizes a surface molecule such as CD19 on leukemia cells. The key thing about the new method are the genetically modified properties of the IL-15, which acts like a kind of security lock. In the MICs, the IL-15 is genetically modified so that it cannot bind to the immune system's killer cells and activate them against cancer until the antibody binds to the cancer cell.
Salih and his colleague Gundram Jung, head of the Experimental Antibody Therapy section at Tübingen University, thus designed a new, modified form of immunocytokines (MICs). They attached interleukin IL-15 to an antibody that recognizes a surface molecule such as CD19 on leukemia cells. The key thing about the new method are the genetically modified properties of the IL-15, which acts like a kind of security lock. In the MICs, the IL-15 is genetically modified so that it cannot bind to the immune system's killer cells and activate them against cancer until the antibody binds to the cancer cell.
“Even with high doses of MICs, we see very little untargeted and hence undesirable activation of killer cells, which in contrast we always see with unmodified immunocytokines even in smaller doses,“ Salih commented. “That means that we can administer higher and hence effective doses without having to worry about dramatic side effects.“ In mice and cell culture experiments, the anti-tumor effect of the new immunotherapeutic agents was so promising that several pharmaceutical companies have already registered their interest. An initial license and cooperation agreement has now been signed with the South Korean biotech company ABL Bio on the production of two MICs.
In the present preclinical studies on cell cultures and mice, the researchers tested MICs against leukemia, lymphomas, and various solid tumors. “But in principle, the newly patented method can be used to equip any cancer-specific antibody with the 'safe' IL-15 and make it more powerful,“ Gundram Jung emphasized, adding that this made treatment with immunocytokines conceivable in patients with very different types of cancer. Over the next 18 months, the researchers and ABL Bio will be concentrating on production of the first two MICs of clinical quality and characterizing their properties in detail. This is to be followed by clinical studies conducted in the Clinical Cooperation Unit Translational Immunology at the DKTK partner site in Tübingen and at other DKTK partner sites. “We are very pleased to have found a really suitable partner from among the many interested parties with whom we can work hard on developing the new immunotherapeutic agents so that we can help cancer patients as soon as possible,“ Helmut Salih remarked.
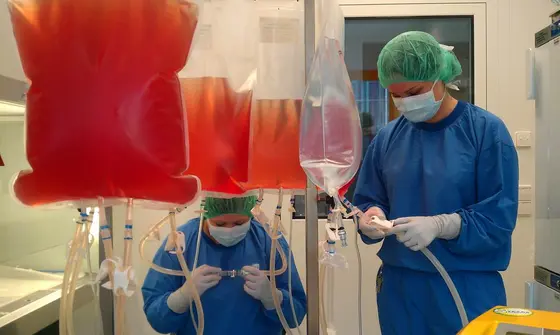
An image for the press release can be found at:
Herstellung-Immuntherapeutika.jpg
Image caption:
Production of immunotherapeutics according to clinical standards in the GMP center of the University Tübingen.
Note on use of images related to press releases
Use is free of charge. The German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ) permits one-time use in the context of reporting about the topic covered in the press release. Images have to be cited as follows: “Source: G. Jung / University Tübingen“.
Distribution of images to third parties is not permitted unless prior consent has been obtained from DKFZ's Press Office (phone: ++49-(0)6221 42 2854, E-mail: presse@dkfz.de). Any commercial use is prohibited.