Molecular patterns are being used more and more frequently in brain tumors to predict the response to cancer therapy and help find the best possible treatment for the patient. “With children's brain tumors, so called medulloblastoma, the prognoses are quite reliable in many cases,“ explains Dr. Marc Remke, who leads the junior group for pediatric neurooncology at the German Cancer Consortium (DKTK) at the University Hospital of Düsseldorf. “If for example the so-called Wnt signaling pathway is activated in the tumor, patients with the most common standard therapies have an excellent chance of recovery.“ Since 2016, these and other molecular classifications of brain tumors have also been recognized by the World Health Organization (WHO).
The prerequisite for the reliability of the methods, however, is clearly determining the genetic tumor profile. Herein lies the challenge, as the cells of a brain tumor often have more differences than similarities, as Marc Remke found together with his Canadian colleagues from the University of Toronto, the Hospital for Sick Children, and the Cancer Agency British Columbia. The team showed for the first time that brain tumors in adults (high grade gliomas) as well as children's brain tumors (medulloblastomas) consist of genetically different regions. The researchers dissected tumor samples from a total of 35 patients and examined the spatial distribution of genetic changes which play a role in tumor development. “The different tumor regions differ by the individual mutation and the copy number of certain genes in the DNA of the cancer cell,“ explained Remke. “Both in the case of child medulloblastomas as well as for as well as with gliomas, two or more biopsies would be necessary in order to determine whether the genetic changes are present in the entire tumor.“
The discovery that brain tumors are not a homogenous unit on a genetic level has considerable consequences for the development of new targeted therapies. “Molecular target structures that are the target of therapeutic agents should be present in all tumor cells, as this lowers the likelihood that resistances will develop. This way we can grab the tumor by the root and spare patients additional biopsies,“ emphasized Remke.
The study identifed the activity of cancer relevant genes, such as the Wnt signaling pathway, as particularly homogeous and therefore promising tumor markers. “With the medulloblastomas, the activity patterns of the genes we examined were comparable in all tumor regions and a single biopsy was enough to form a reliable prognosis,“ said Remke.
Remke is confident that the results of the study will contribute to greater consideration of the heterogeneity of brain tumors with respect to the choice of the correct marker. Currently, the researchers are studying whether there are further molecular changes in cancer which occur in all tumor regions. “We have early indications that so-called epigenetic factors, chemical groups in the DNA, could be interesting for the diagnostics of brain tumors,“ said Remke, summarizing initial findings.
A Sorana Morrissy. et. al.: Spatial heterogeneity in medulloblastoma. In: Nature Genetics (10. April 2017)
doi:10.1038/ng.3838 (http://www.nature.com/ng/journal/v49/n5/full/ng.3838.html)
A picture for the press release is available at:
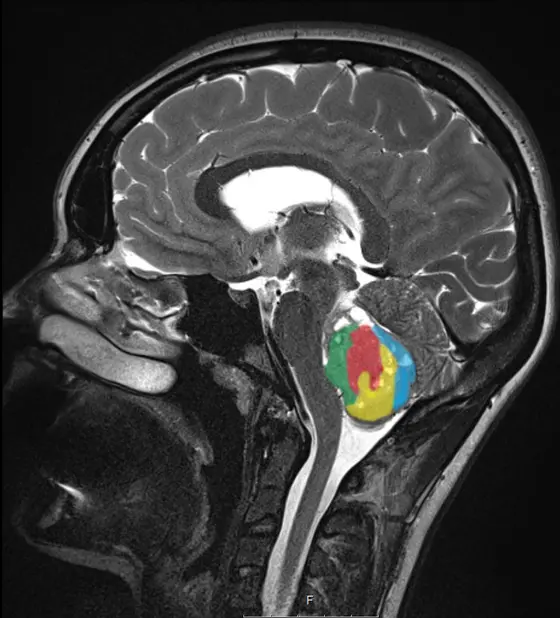
medulloblastoma_colored.jpg
Caption: Medulloblastomas (yellow circle) are one of the most common malignant tumors for children.
Note on use of images related to press releases
Use is free of charge. The German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ) permits one-time use in the context of reporting about the topic covered in the press release. Images have to be cited as follows: “Source: Marc Remke / Universitätsklinikum Düsseldorf“.
Distribution of images to third parties is not permitted unless prior consent has been obtained from DKFZ's Press Office (phone: ++49-(0)6221 42 2854, E-mail: presse@dkfz.de). Any commercial use is prohibited.
* The German Cancer Consortium (DKTK) is a joint long-term initiative involving the German Federal Ministry of Education and Research (BMBF), participating German states and the German Cancer Research Center (DKFZ) and was established as one of six German Health Research Centres (DZGs). As DKTK's core center the DKFZ works together with research institutions and hospitals in Berlin, Dresden, Essen/Düsseldorf, Frankfurt/Mainz, Freiburg, Munich, Heidelberg and Tübingen to create the best possible conditions for clinically oriented cancer research. The consortium promotes interdisciplinary research at the interface between basic research and clinical research, as well as clinical trials for innovative treatments and diagnostic methods. Another key focus of the consortium's work is on developing research platforms to speed up the application of personalized cancer treatments and to improve the diagnosis and prevention of cancer.
More information is available at www.dktk.org