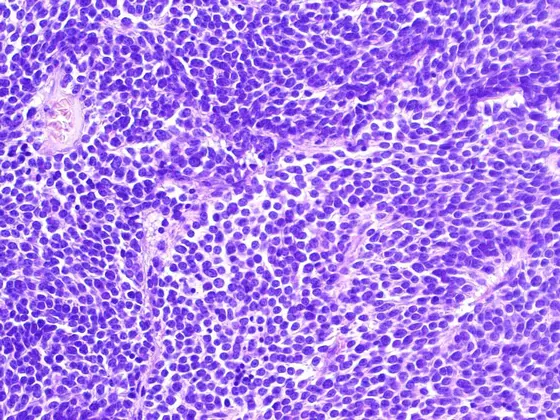
Many childhood brain tumors arise from extremely immature and undifferentiated cells of the central nervous system (CNS) and are therefore referred to as embryonal tumors. These include, for example, medulloblastomas, which always occur in the cerebellum. A large part of embryonal brain tumors that are located above the cerebellum are grouped as primitive neuroectodermal tumors of the central nervous system (CNS PNET). About 10 children and 40 adults are diagnosed with this type of cancer in Germany every year. These brain tumors grow extremely rapidly and aggressively and are difficult to treat.
“More recent studies have revealed that PNET are a group of heterogeneous cancers," says Andrey Korshunov, a neuropathologist who works at the DKFZ and Heidelberg University Hospital. “However, precise diagnosis is difficult because there are no molecular markers and in histologic differentiation of tumor tissue under the microscope there are overlaps with many other types of brain cancer."
In order to facilitate better classification of these dangerous tumors and, thus, more precise and eventually more successful treatment for each individual patient, an international research group led by Marcel Kool from the DKFZ and David Ellison from St. Jude, (Memphis, Tenn., USA) launched a large-scale study in which researchers conducted a comprehensive molecular and histologic analysis of tissue samples from over 300 CNS PNET cases.
In the first step, the investigators mapped the distribution of methyl labels in the tumor genomes. By comparing these methylation profiles with reference tumors, they recognized that approximately two thirds of the presumed CNS PNET could be grouped with other known CNS tumor types. In many cases, this observation was additionally supported by histologic re evaluation of the tumor tissue.
“This result shows how important molecular analysis of these primitive tumors is. In many cases, our new classification suggests completely different treatment options," says pediatrician and molecular geneticist Dominik Sturm, who is one of the first authors of the article. At St. Jude, the study was directed by first author and neuropathologist Brent Orr.
The researchers were able to classify the bulk of the remaining tumors in four new, previously unknown tumor types, which exhibit significant differences as to patients' age and gender as well as clinical course. Further analyses such as gene activity profiles, determining the copy number of chromosomes as well as DNA sequencing revealed a characteristic genetic alteration for each of the four new tumor types in addition to their specific DNA methylation profiles. In contrast, it was difficult to distinguish these groups based solely on their histologic features.
“Based on the molecular tumor profiles, we can assign affected patients to future clinical trials that make sense for them," Sturm explains. "The tumors in the four newly described groups differ from all previously known brain tumors markedly enough to speak of new tumor types. We expect that they also vary in their response to chemotherapy and targeted drugs." The molecular analysis has already yielded first clues about potential targets in the individual tumor groups.
This research shows the importance of international collaborations in the study of rare types of cancer. This comprehensive study would not have been possible without the linkage of two of the world’s largest research centers with a focus on pediatric oncology, the DKFZ in cooperation with Heidelberg University Hospital and St. Jude.
The project was supported, among other sources, by German Cancer Aid (Deutschen Krebshilfe), the German Childhood Cancer Foundation (Deutsche Kinderkrebsstiftung), the Federal Ministry of Education and Research (BMBF) and ALSAC (Memphis, USA).
Dominik Sturm, Brent A. Orr, Umut H. Toprak, Volker Hovestadt, David T. W. Jones, David Capper, Martin Sill, Ivo Buchhalter, Paul A. Northcott, Irina
Leis, Marina Ryzhova, Christian Koelsche, Elke Pfaff, Sariah J. Allen, Gnanaprakash Balasubramanian, Barbara C. Worst, Kristian W. Pajtler, Sebastian Brabetz, Pascal D. Johann, Felix Sahm, Jüri Reimand, Alan Mackay, Diana M. Carvalho, Marc Remke, Joanna J. Phillips, Arie Perry, Cynthia Cowdrey, Rachid Drissi, Maryam Fouladi, Felice Giangaspero, Maria Łastowska, Wiesława Grajkowska, Wolfram Scheurlen, Torsten Pietsch, Christian Hagel, Johannes Gojo, Daniela Lötsch, Walter Berger, Irene Slavc, Christine Haberler, Anne Jouvet, Stefan Holm, Silvia Hofer, Marco Prinz, Catherine Keohane, Iris Fried, Christian Mawrin, David Scheie, Bret C. Mobley, Matthew J. Schniederjan, Mariarita Santi, Anna M. Buccoliero, Sonika Dahiya, Christof M. Kramm, André O. von Bueren, Katja von Hoff, Stefan Rutkowski, Christel Herold-Mende, Michael C. Frühwald, Till Milde, Martin Hasselblatt, Pieter Wesseling, Jochen Rößler, Ulrich Schüller, Martin Ebinger, Jens Schittenhelm, Stephan Frank, Rainer Grobholz, Istvan Vajtai, Volkmar Hans, Reinhard Schneppenheim, Karel Zitterbart, V. Peter Collins, Eleonora Aronica, Pascale Varlet, Stephanie Puget, Christelle Dufour, Jacques Grill, Dominique Figarella-Branger, Marietta Wolter, Martin U. Schuhmann, Tarek Shalaby, Michael Grotzer, Timothy van Meter, Camelia-Maria Monoranu, Jörg Felsberg, Guido Reifenberger, Matija Snuderl, Lynn Ann Forrester, Jan Koster, Rogier Versteeg, Richard Volckmann, Peter van Sluis, Stephan Wolf, Tom Mikkelsen, Amar Gajjar, Kenneth Aldape, Andrew S. Moore, Michael D. Taylor, Chris Jones, Nada Jabado Matthias A. Karajannis, Roland Eils, Matthias Schlesner, Peter Lichter, Andreas von Deimling, Stefan M. Pfister, David W. Ellison, Andrey Korshunov, and Marcel Kool:
New Brain Tumor Entities Emerge from Molecular Classification of CNS-PNETs, CELL 2016, DOI: 10.1016/j.cell.2016.01.015