Incurable astrocytomas, including the particularly malignant glioblastomas, diffusively grow like mycelium into healthy brain tissue. Therefore, these tumors cannot be completely removed by surgery and invariably start growing again at some point despite intensive treatment. They appear to have effective resistance mechanisms.
In their latest publication, scientists co-working with Frank Winkler from the Clinical Cooperation Unit (CCU) “Neurooncology" of the DKFZ and Heidelberg University Hospital, describe a striking feature of astrocytoma cells: They form extremely thin and long extensions of their cellular membrane, which they use to constantly scan the healthy brain, thus invading and colonizing it. As the tumor grows, the cancer cells use these extensions to interconnect to a large network where they communicate intensively and via long distances, making astrocytomas appear like highly complex, organ-like entities. “Our first thought was: this looks like the formation of a new brain within the existing one," Winkler said. “The tumor cells were interconnected in a network that resembles the ones we know of neurons and other cell types in the brain."
For up to one year, the researchers observed the growth of human glioblastoma cells that they had transferred to mice. They used a special microscopy technique that facilitates insights into the brain’s deep zones. In this way, they discovered that the cancer cells exchanged molecules via their membrane microtubes which they also used as communication channels.
The investigators also found this network of tumor microtubes in tissue samples from brain cancer patients. The more the cancer cells were interconnected, the more malignant and resistant the tumor subtype was.
The scientists therefore hypothesized that the tumor microtube networks must be linked to therapy resistance. They observed that the tumors in fact recognize damage to the network and repair it immediately. Radiation therapy – the standard treatment in glioblastoma – fails to kill mainly the tumor cells that are part of the network, whereas cancer cells outside the network die.
How do the tumor cells form these extraordinary membrane extensions? An analysis of the gene activities in tumor tissue from 250 brain cancer patients provided a clue. For building their network, the cancer cells make use of specific molecular signaling pathways that are normally active during early development of the nervous system. Experiments in which the scientists blocked these pathways in mice showed that the animals subsequently developed smaller tumors with fewer interconnections that responded very sensitively to radiotherapy.
“The resistance of astrocytomas, particularly glioblastomas, against all types of therapy is an enormous problem," says Wolfgang Wick, who heads the CCU as well as the Neurology Department of Heidelberg University Hospital. “For the first time, our results show a long sought-after new approach toward breaking this resistance and thus enabling us eventually to enhance the treatment efficacies of these tumors. The results also explain why a specific subtype of brain cancer responds much better to therapy. Their capability of building networks seems to be limited." Matthias Osswald, the article’s first author, adds: “Even though this discovery does not immediately enable us to offer a new treatment to our brain tumor patients, it does show the direction that therapy development should take: we have to destroy the malignant network."
Matthias Osswald, Erik Jung, Felix Sahm, Gergely Solecki, Varun Venkataramani, Jonas Blaes, Sophie Weil, Heinz Horstmann, Benedikt Wiestler, Mustafa Syed, Lulu Huang, Miriam Ratliff, Kianush Karimian Jazi, Felix T. Kurz, Torsten Schmenger, Dieter Lemke, Miriam Gömmel, Martin Pauli, Yunxiang Liao, Peter Häring, Stefan Pusch, Verena Herl, Christian Steinhäuser, Damir Krunic, Mostafa Jarahian, Hrvoje Miletic, Anna S. Berghoff, Oliver Griesbeck, Georgios Kalamakis, Olga Garaschuk, Matthias Preusser, Samuel Weiss, Haikun Liu, Sabine Heiland, Michael Platten, Peter E. Huber, Thomas Kuner, Andreas von Deimling, Wolfgang Wick und Frank Winkler: Brain tumor cells interconnect to a functional and resistant network. Nature 2015, DOI: 10.1038/nature16071
Link to Nature “News and Views": http://www.nature.com/nature/journal/vaop/ncurrent/full/nature15649.html
A picture is available at:
vernetztes-Glioblastom.jpg
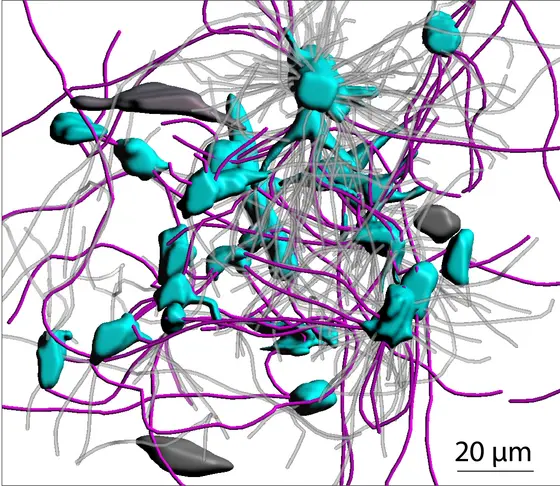
Caption: 3D-Illustration of a glioblastoma: Interconnected tumor cells (blue) with the connecting microtubes (pink). Tumor cells and microtubes outside the network are grey (Source: Nature).