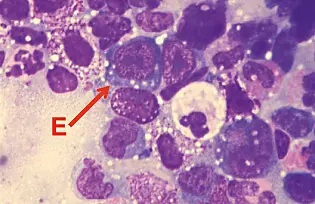
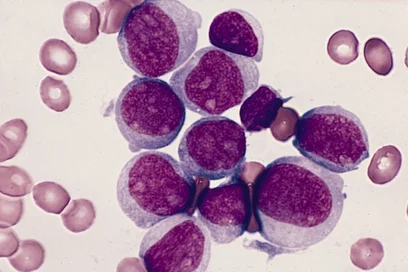
Patients suffering from a myelodysplastic disorder (MDS) exhibit highly unusual blood counts. Their hematopoietic stem cells – the source of blood – are defective, and they do not mature into functioning blood cells. As a result, MDS patients suffer from general physical weakness, internal bleeding and severe infections. About one third of MDS cases progress into acute myeloid leukemia, a type of blood cancer that is difficult to treat.
Several attempts have been made to transplant stem cells from MDS patients to mice, in hopes that the defective cells would multiply in the marrow and researchers could study their abnormal maturation. However, all these attempts have failed so far. “We had clues suggesting that the blood stem cells from MDS patients need specific conditions in the bone marrow in order to settle there,“ says Prof. Dr. Andreas Trumpp, who heads the Division of Stem Cells and Cancer at DKFZ and the Heidelberg Institute for Stem Cell Technology and Experimental Medicine (HI-STEM), supported by the DKFZ and the Dietmar Hopp Foundation. “Now we have been able to prove this in a collaboration with Wolf-Karsten Hofmann and Daniel Nowak and their groups at the Department of Hematology and Oncology of the University Medical Centre Mannheim."
In their recent work, the stem cell researchers turned to a trick: They transplanted the blood-forming cells of MDS patients along with so-called “niche cells“ from the same person. Niche cells, or mesenchymal stromal cells, to use scientific terminology, settle predominantly in the bone marrow and produce a number of protein factors required for the survival of hematopoietic stem cells. The niche they form is a type of micro-environment in which stem cells flourish.
It turned out that only the niche cells taken from a patient, and not from healthy donors, led to a successful transplantation. A comparison of healthy niche cells with those taken from the patient revealed numerous genetic and molecular differences: a patient's cells produce different factors that promote the settling-in of transplanted MDS blood stem cells.
What causes this difference? Might it be caused by the abnormal blood stem cells themselves? Raising both cell types together in one culture dish, the scientists discovered that defective MDS blood stem cells are able to reprogram the niche cells of healthy donors; these subsequently begin producing excessive quantities of growth factors which, in turn, promote the survival of MDS stem cells.
“MDS blood stem cells and their niche apparently have an impact on each other, and this further aggravates the disorder in the formation of blood,“ says Dr. Hind Medyouf, first author of the publication. “This work provides the first indications that when the niche cells are reprogrammed by cells with the MDS defect, they produce protein factors that particularly promote the abnormal development of MDS stem cells, but fail to promote healthy blood stem cell development.“ Hence, the abnormal MDS blood stem cells and those of the niche form a functional unit that drives the disease further in a vicious cycle.
The new discovery of these interactions suggests a potential to use drugs or antibodies to inhibit growth factors that are excessively produced by the reprogrammed niche cells. Thus, the researchers hope to break the cycle and interfere early on in order to prevent MDS from progressing into leukemia.
Hind Medyouf, Maximilian Mossner, Johann-Christoph Jann, Florian Nolte, Simon Raffel, Carl Herrmann, Amelie Lier, Christian Eisen, Verena Nowak, Bettina Zens, Katja Müdder, Corinna Klein, Julia Obländer, Stephanie Fey, Jovita Vogler, Alice Fabarius, Eva Riedl, Henning Roehl, Alexander Kohlmann, Marita Staller, Claudia Haferlach, Nadine Müller, Thilo John, Uwe Platzbecker, Georgia Metzgeroth, Wolf-Karsten Hofmann, Andreas Trumpp and Daniel Nowak: Myelodysplastic cells in patients re-program mesenchymal stromal cells to establish a transplantable stem cell-niche disease unit. Cell Stem Cell 2014, DOI: 10.1016/j.stem.2014.02.014