Translationale Radioonkologie
- Bildgebung und Radioonkologie
- Klinische Kooperationseinheit

Prof. Dr. Amir Abdollahi
Die Strahlentherapie ist ein integraler Bestandteil der Krebstherapie. Eine neue und vielversprechende Entwicklung im Bereich der Strahlentherapie ist die Einführung der Behandlung mit geladenen Teilchen, z.B. Protonen und schweren Ionen wie Kohlenstoff, in die Klinik. Die speziellen physikalischen Eigenschaften der Teilchenbestrahlung und die hervorragenden klinischen Daten haben zur Entstehung einer weltweit einzigartigen klinischen Therapieanlage in Heidelberg geführt.
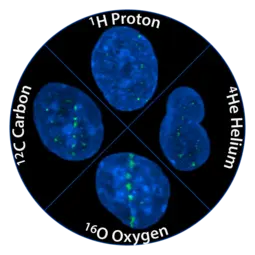
Unsere Forschung
Während empirisch- phänomenologische Daten eine erhöhte biologische Effizienz der Teilchentherapie postulieren, gibt es noch keine systematische molekularbiologische Analyse dieser Strahlenqualitäten. Der Forschungsschwerpunkt dieser Arbeitsgruppe ist die molekulare Untersuchung der Strahlen-Wechselwirkungen unterschiedlicher Strahlenqualitäten (Photon-, Proton- und Kohlenstoff- Teilchen) mit Normal- bzw. Tumorgewebe. Die Translationale Radioonkologie besitzt bereits Expertise auf dem Gebiet der Tumor-Angiogenese und des Tumor-Microenvironments sowie der Wechselwirkungen dieser mit Photonen-Bestrahlung. Wir konnten zeigen, dass Tumoren ihr Gefäßsystem vor Strahlenschäden schützen, indem sie pro-angiogene und andere Überlebensfaktoren produzieren. Die Hemmung dieser parakrinen Tumor-Wirt-Kommunikation führt zu einer wesentlich verbesserten Effizienz der Strahlentherapie. Somit bildet die Tumor-Gefäss- und Tumor-Stroma-Kommunikation ein wichtiges Ziel, um die erworbene Resistenz von Tumoren gegenüber Strahlen- und Chemotherapie zu verhindern. Dieses Konzept wird gerade im Rahmen multimodaler Therapien bestehend aus Radiotherapie, Chemotherapie und Antiangiogenese in klinischen Studien in Heidelberg und weltweit getestet. Ziel der Gruppe ist die Ausweitung dieser Arbeiten auf die neuen Strahlenqualitäten, die nun im Heidelberger Ionen-Therapie Zentrum (HIT) verfügbar sind. Ein weiteres Ziel ist der Aufbau einer integrativen Molekularbiologie-Plattform zur Identifizierung der Zell-Zell-Interaktionen und der intrazellulären Signalwege/ -netzwerke, die durch Protonen- und Kohlenstoffbestrahlung aktiviert werden. Hierfür werden molekulare Untersuchungen des Genoms, Transkriptoms, Epigenoms und Proteoms sowie micro-RNA Analysen angewandt.
Die erfolgreiche Translation von molekularbiologisch erworbenen Kenntnissen in die Klinik ist eine Stärke unserer Arbeitsgruppe, welche nun, durch die Eingliederung der Nachwuchsgruppe in das Nationale Centrum für Tumorerkrankungen (NCT) Heidelberg, mit Unterstützung der Radiologischen Universitätsklinik und des Deutschen Krebsforschungszentrums (DKFZ) intensiviert werden soll.
Ausgewählte wissenschaftliche Highlights der Abteilung:
- Die Rolle der interzellulären Kommunikation bei der Entfaltung der Wirkung der Strahlentherapie.
Tumor-Mikromilieu-Wechselwirkungen, u.a. Tumor-Angiogenese, Tumor-Fibrogenese, Rekrutierung von Zellen aus dem Knochenmark.
Ziel: Identifizierung von wichtigen Zielstrukturen zur Erhöhung der Strahleneffizienz bzw. Schonung des Normalgewebes
- Integrative Radiobiologie der Photonen und Partikeltherapie (Protonen und Kohlenstoffionen).
Ziel: Entschlüsselung der Strahlentherapie-induzierten Veränderungen des Genoms, Transkriptoms (mRNA, miRNA) und Proteoms.
- Mechanismus der Tumor-Resistenz gegen multimodale Therapien bestehend aus Radiotherapie, Chemotherapie und „targeted“ (zielgerichteten) Therapien
Ziel: Verbesserung der Therapieeffizienz durch Resensibilisierung von Tumoren, Entwicklung präklinischer Rationalen für innovative multimodale Therapiekombinationen.
- Untersuchung von „dormanten“ Tumoren, die u.a. als minimal residual disease bzw. Mikrometastasen nach erfolgreicher lokaler Therapie zurückbleiben können und des „angiogenen switch“, der zu einer Konversion von dormanten zu malignen (symptomatischen) Tumoren führt.
Ziel: Entdeckung von dormanten Tumoren zum frühestmöglichen Zeitpunkt, Prävention bzw. Reversion des angiogenen switch.
- Entschlüsselung molekularer Mechanismen, die zu lokaler Invasion und Metastasierung von Tumoren beitragen, zwei der wichtigsten Faktoren des Therapieversagens nach Strahlentherapie.
Ziel: Modulation dieser Mechanismen zwecks Verbesserung der Überlebensrate nach erfolgreicher lokaler Strahlentherapie. Herstellung von „nicht-permissiven“ Tumor-Nischen.
- Identifikation von Therapie-Prädiktoren und Surrogatmarkern mittels genomweiter Untersuchungen des peripheren Bluts, Tumorgewebes und Tumor-Mikromilieus.
Ziel: Patienten-Stratifikation und molekulares Monitoring des Therapieerfolgs.
- Identifizierung von Strahlen-induzierten Tumorgefäß-Endothelzell-Oberflächenmarkern.
Ziel: In-vivo Biodosimetrie zwecks verbesserter Bildgebung und Strahlenplanung sowie „dose painting“ für gezielte endogene Radiotherapie bzw. „drug delivery“.
Projekte
Wir verbessern die Partikel-Radiotherapie, indem wir biophysikalische Unsicherheiten reduzieren und modernste Bildgebung, Multi-Ionen-Therapiepläne und neue Bestrahlungsmethoden wie die Spot-Scanning-Hadron Arc- (SHArc-)Therapie integrieren. Unsere Arbeit umfasst die präzise Tumorabgrenzung durch multimodale Bildgebung, KI-gestützte Radiomik und biophysikalische Modellierung. Zudem erforschen wir die FLASH-Partikeltherapie, um gesundes Gewebe gezielt zu schonen und gleichzeitig die Tumorkontrolle zu verbessern – insbesondere bei strahlenresistenten Tumoren wie Glioblastomen. Unser Ziel ist es, die Wirksamkeit der Behandlung zu maximieren und gleichzeitig Schäden am umliegenden gesunden Gewebe zu minimieren.
Wir untersuchen, wie die Strahlentherapie das Tumor-Immunmikromilieu (TIME) beeinflusst und wie diese Erkenntnisse für eine verbesserte Krebsbehandlung genutzt werden können. Unser Fokus liegt auf der Optimierung der Immunaktivierung durch die Kombination von Strahlentherapie mit TGF-β-Inhibition und Checkpoint-Blockade, um immunologisch „kalte“ Tumoren in therapieresponsive „heiße“ Tumoren umzuwandeln. Wir erforschen zentrale immunmodulierende Faktoren, untersuchen Abscopaleffekte und entwickeln personalisierte in-situ-Tumorimpfstrategien zur Verbesserung der Therapieantwort.
Durch die Integration von molekularen, zellulären und bildgebenden Daten entwickeln wir Biomarker und prädiktive Modelle zur individualisierten Anpassung der Strahlentherapie. Ein besonderer Schwerpunkt liegt auf der Stratifizierung von Patienten mit Kopf-Hals-Tumoren anhand von Tumorhypoxie- und Immunprofilen, um Therapieintensivierung oder -deeskalation gezielt zu steuern. Darüber hinaus wollen wir die Tumorevolution unter Strahlentherapie vorhersagen und neue biologische Zielstrukturen identifizieren, um die Behandlung sowohl am Primärtumor als auch an metastasierten Tumoren zu optimieren.
-

Prof. Dr. Amir Abdollahi
-
Claudia Rittmüller
-
Dr. Bouchra Tawk
-
Dr. Julian Schlegel
-
Dr. Jennifer Furkel
-
Allegra Gerharz
-
Matilde Recusani
-
Neele Haxel
Ausgewählte Publikationen
Tawk B, Rein K, Schwager C, Knoll M, Wirkner U, Hörner-Rieber J, Liermann J, Kurth I, Balermpas P, Roedel C, Linge A, Loeck S, Lohaus F, Tinhofer I, Krause M, Stuschke M, Grosu AL, Zips D, Combs SE, Belka C, Stenzinger A, Herold-Mende C, Baumann M, Schirmacher P, Debus J, Abdollahi A
Dokic I, Meister S, Bojcevski J, Tessonnier T, Walsh D, Knoll M, Mein S, Tang Z, Vogelbacher L, Rittmueller C, Moustafa M, Krunic D, Brons S, Haberer T, Debus J, Mairani A, Abdollahi A
Adeberg S, Knoll M, Koelsche C, Bernhardt D, Schrimpf D, Sahm F, König L, Harrabi SB, Hörner-Rieber J, Verma V, Bewerunge-Hudler M, Unterberg A, Sturm D, Jungk C, Herold-Mende C, Wick W, von Deimling A, Debus J, Rieken S, Abdollahi A
Lan Y, Moustafa M, Knoll M, Xu C, Furkel J, Lazorchak A, Yeung TL, Hasheminasab SM, Jenkins MH, Meister S, Yu H, Schlegel J, Marelli B, Tang Z, Qin G, Klein C, Qi J, Zhou C, Locke G, Krunic D, Derner MG, Schwager C, Fontana RE, Kriegsmann K, Jiang F, Rein K, Kriegsmann M, Debus J, Lo KM, Abdollahi A
Tawk B, Wirkner U, Schwager C, Rein K, Zaoui K, Federspil PA, Adeberg S, Linge A, Ganswindt U, Hess J, Unger K, Tinhofer I, Budach V, Lohaus F, Krause M, Guberina M, Stuschke M, Balermpas P, Rödel C, Grosu AL, Schäfer H, Zips D, Combs SE, Pigorsch S, Zitzelsberger H, Baumeister P, Kirchner T, Bewerunge-Hudler M, Weichert W, Hess J, Herpel E, Belka C, Baumann M, Debus J, Abdollahi A
Chiblak S, Tang Z, Lemke D, Knoll M, Dokic I, Warta R, Moustafa M, Mier W, Brons S, Rapp C, Muschal S, Seidel P, Bendszus M, Adeberg S, Wiestler OD, Haberkorn U, Debus J, Herold-Mende C, Wick W, Abdollahi A
Zhou C, Moustafa MR, Cao L, Kriegsmann M, Winter M, Schwager C, Jones B, Wang S, Bäuerle T, Zhou PK, Schnölzer M, Weichert W, Debus J, Abdollahi A
Abdollahi A, Folkman J
Heidelberger Institut für Radioonkologie (HIRO)
Unsere Abteilung ist Teil des Heidelberger Instituts für Radioongologie (HIRO).

Kontaktieren Sie uns

