Neurons promote growth of brain tumor cells
Joint press release by Heidelberg University Hospital and the German Cancer Research Center
In a current paper published in the journal Nature, Heidelberg-based researchers and physicians describe how neurons in the brain establish contact with aggressive glioblastomas and thus promote tumor growth / New tumor activation mechanism provides starting points for clinical trials
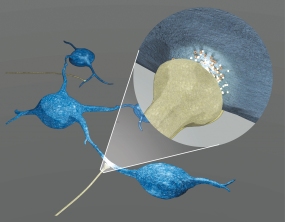
Graphic presentation of the newly discovered mechanism by which neurons (brown) promote growth of brain tumor cells (blue).
© Tanev/ Heidelberg University Hospital
Neurons transmit their signals to each other via synapses, fine cell projections with terminals that contact another neuron. Researchers and physicians at Heidelberg University Hospital, Heidelberg Medical Faculty, and the German Cancer Research Center (DKFZ) have now discovered that neurons in the brain form these kinds of direct cell-to-cell contacts with tumor cells of aggressive glioblastomas too, thus transmitting impulses to the cancer cells. The tumor benefits from this input: The activation signals are probably a driving force behind the tumor growth and the invasion of healthy brain tissue by tumor cells, as Frank Winkler, Thomas Kuner, and their teams discovered using special imaging methods. But there is also some good news: Certain substances can block the signal transmission in animal experiments. The results have just been published online in the journal Nature.
Networks of neurons and tumor cells
Glioblastomas invade the healthy brain in a diffuse pattern like a fungal network. As a result, they cannot be completely removed by surgery, and they also survive intensive chemotherapy and radiotherapy. Glioblastomas are thus among the most dangerous tumors in humans; the average survival time is 15 months following the initial diagnosis.
In 2015, the team led by Frank Winkler, head of the Research Group Experimental Neurooncology in the Clinical Cooperation Unit Neurooncology, discovered a cause of this resistance to treatment: The glioblastoma cells are connected to one another through long cell protrusions. They communicate through these connections, exchange substances that are relevant for their survival, and thus protect themselves from treatment-related damage. The current findings add a further piece of the puzzle to our understanding of this type of cancer: The tumor cells are not only interconnected in the brain like neurons; they also receive direct signals from them, explained Winkler, whose research group is affiliated with the University Hospital and the DKFZ.
The researchers observed the growth of human glioblastomas that they had transferred to mice, and studied cell cultures with human neurons and tumor cells, and tissue samples from patients. To do so, they used a wide range of modern microscopy methods, which provide detailed three-dimensional images of the connections only micrometers large between neurons and tumor cells as well as showing their molecular structure and signals within the cells. Electrical recordings from tumor cells revealed electrical currents generating from the synaptic connections, which form the starting point for further processing of these signals in the tumor cells. We were able to show that signal transmission from neurons to tumor cells does in fact work like stimulating synapses between the neurons themselves, added Thomas Kuner, Director of the Department of Functional Neuroanatomy at the Institute for Anatomy and Cell Biology, where the synaptic connections were first discovered by Varun Venkataramani. This project began with an observation in basic research. In close cooperation with our clinical partners, it has led to conceptually new insights which will allow new treatment approaches to be developed using targeted translational research.
A fatal mechanism but one that opens up new avenues for treatment
How exactly activation of the tumor cell ultimately leads to increased tumor growth and invasion of healthy areas of the brain by the glioma cells has yet to be clarified. It is clear that this mechanism can be blocked in animals, however. Possible methods include a significant reduction of brain activity (for example under general anesthesia), pharmacological interventions that interrupt binding of the neurotransmitters on the AMPA receptor, or blocking the AMPA receptor using genetic engineering. In all these cases, tumor spread became slower in animal experiments. This mechanism is therefore an extremely interesting approach for drug development and future drug treatments, neurooncologist Winkler emphasized. Suitable substances have in fact already been approved that block the AMPA receptor and are used to treat other neurological diseases. These substances are promising candidates for clinical trials.
The new results not only show what makes glioblastomas so aggressive, but also how they could be stopped. That is highly relevant from a translational point of view and paves the way for clinical studies, commented Wolfgang Wick, Medical Director of the Neurology Department at Heidelberg University Hospital and head of the Clinical Cooperation Unit Neurooncology at DKFZ. We are also extremely pleased that the work of our junior researcher Varun Venkataramani, who also works in clinical practice, has been acknowledged by a publication in such a prestigious journal as ,Nature.
The relevance of the results from Heidelberg has been confirmed by a paper from Stanford University, California, USA: Michelle Monje and her research team also found synaptic connections between neurons and tumor cells in currently untreatable pediatric brain tumors and also observed the treatment effects reported by the Heidelberg-based researchers. Both papers are being published in Nature simultaneously.
Contact:
Frank Winkler
Department of Neurology, Heidelberg University Hospital
Clinical Cooperation Unit Neurooncology, German Cancer Research Center
Tel.: +49 6221 567504
Email: frank.winkler@med.uni-heidelberg.de
Thomas Kuner
Director, Department of Functional Neuroanatomy
Institute for Anatomy and Cell Biology
Tel. +49 6221 548678
Email: thomas.kuner@uni-heidelberg.de
Original publication:
https://rdcu.be/bRnKb
DOI: 10.1038/s41586-019-1564-x
Nature News:
https://www.nature.com/articles/d41586-019-02792-1
https://www.nature.com/articles/d41586-019-02746-7
Further information:
https://www.klinikum.uni-heidelberg.de/neurologische-klinik/neurologie-und-poliklinik/forschung/neurooncology/
https://www.dkfz.de/en/neuroonkologie/AG_Winkler.html
http://www.ana.uni-heidelberg.de/index.php?id=130
About DKFZ
The German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ) with its more than 3,000 employees is the largest biomedical research institution in Germany. At DKFZ, more than 1,300 scientists investigate how cancer develops, identify cancer risk factors and endeavor to find new strategies to prevent people from getting cancer. They develop novel approaches to make tumor diagnosis more precise and treatment of cancer patients more successful. DKFZs Cancer Information Service (KID) provides individual answers to all questions about cancer for patients, the general public, and health care professionals. Jointly with partners from Heidelberg University Hospital, DKFZ runs the National Center for Tumor Diseases (NCT) located in Heidelberg and Dresden, and, also in Heidelberg, the Hopp Childrens Cancer Center (KiTZ). In the German Cancer Consortium (DKTK), one of six German Centers for Health Research, DKFZ maintains translational centers at seven university partnering sites. Combining excellent university hospitals with high-profile research at a Helmholtz Center at the NCT and DKTK sites is an important contribution to the endeavor of translating promising approaches from cancer research into the clinic in order to improve the chances of cancer patients. DKFZ is a member of the Helmholtz Association of National Research Centers, with ninety percent of its funding coming from the German Federal Ministry of Education and Research and the remaining ten percent from the State of Baden-Württemberg.
About Heidelberg University Hospital and the Medical Faculty of Heidelberg University
Heidelberg University Hospital is one of the largest and most prestigious medical centers in Germany. The Medical Faculty of Heidelberg University belongs to the internationally most renowned biomedical research institutions in Europe. Both institutions have the common goal of developing new therapies and implementing them rapidly for patients. With about 13.000 employees, training and qualification is an important issue. Every year, around 65,000 patients are treated on an inpatient basis, 56.000 day patients and around 1.000.000 outpatient cases are treated in more than 50 clinics and departments with 2000 beds. Currently, about 3,700 future physicians are studying in Heidelberg; the reform Heidelberg Curriculum Medicinale (HeiCuMed) is one of the top medical training programs in Germany.

